Endometriosis and Pain: Navigating Relief with Confidence
Endometriosis and Pain: Navigating Relief with Confidence
Endometriosis is a chronic condition that affects 1 in 10 women and people with uteruses in the United States, yet it remains widely misunderstood. Too often, the pain associated with endometriosis is dismissed or misdiagnosed, leaving many to suffer in silence without the answers or relief they deserve. At UpLift Physical Therapy in San Antonio, we help women find effective endometriosis pain relief through pelvic floor therapy and holistic care.
In this post, we’ll break down what endometriosis is, how it impacts the body, and the role pelvic floor dysfunction plays in the pain cycle—because understanding your body is the first step toward finding relief.
What is Endometriosis and How Does It Cause Pain?
Endometriosis occurs when tissue similar to the lining of the uterus (the endometrium) grows outside the uterus. These growths, called endometrial implants, can develop on the ovaries, fallopian tubes, the outer surface of the uterus, and even beyond the reproductive organs, such as the intestines and bladder. Unlike the uterine lining, which sheds during menstruation, these growths have no way to exit the body, leading to chronic inflammation, adhesions, and scar tissue formation.
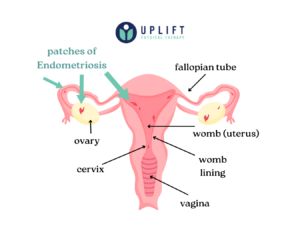
Understanding where endometriosis affects the body can help in managing symptoms and seeking targeted treatment.
Common Endometriosis Symptoms
Endometriosis symptoms can vary widely, but some of the most common include:
- Pelvic pain – This can be chronic or cyclical, often worsening around menstruation.
- Painful periods (dysmenorrhea) – Intense cramping that doesn’t always respond to typical pain relief methods.
- Pain with intercourse (dyspareunia) – Deep, aching, or sharp pain during or after sex.
- Infertility – Scarring and inflammation can interfere with reproductive function.
- Gastrointestinal (GI) and urinary symptoms – Bloating, constipation, painful bowel movements, and bladder pain—especially if endometriosis affects the intestines or bladder.
It’s important to note that the impact of endometriosis goes beyond physical discomfort. Chronic pain and fatigue can limit work, social activities, and relationships, making even everyday tasks feel overwhelming.
If this sounds familiar, know that you’re not alone—and that relief is possible.
Why Endometriosis Pain Feels Different
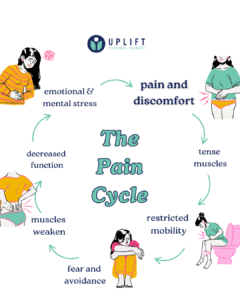
The endometriosis pain cycle is real—start breaking the cycle with targeted therapy and strategies for relief.
Unlike muscle strain or acute injuries, endometriosis-related pain is often deep, burning, and persistent. It isn’t always localized to one spot—it can radiate to the lower back, pelvis, hips, and even legs. Additionally, because endometriosis involves inflammation and adhesions, everyday functions like movement, digestion, and bladder control can trigger pain, making it different from conditions that solely affect muscles or nerves.
How Inflammation and Scar Tissue Affect Endometriosis Pain
Endometriosis triggers a chronic inflammatory response, meaning the body stays in a prolonged state of irritation, leading to ongoing swelling and discomfort. Over time, the body attempts to heal by forming adhesions—bands of scar tissue that can:
- cause tightness
- restrict movement
- impact digestion and bladder function
While these changes can be frustrating, relief is possible. Reducing inflammation through movement, breathwork, and gentle therapies can improve comfort, support mobility, and help the body function more smoothly.
The Link Between Endometriosis and Pelvic Floor Dysfunction
The persistent pain and inflammation caused by endometriosis often lead to pelvic floor muscle dysfunction. In response to pain, the pelvic floor muscles may become overly tight, creating additional symptoms such as:
- Difficulty relaxing the pelvic floor, leading to pain with intercourse or bowel movements.
- Increased urinary urgency – feeling the constant urge to go, even when the bladder isn’t full.
- Frequent urination – needing to use the restroom every two hours or less.
You can read more about pelvic floor muscle tension in our blog here!
The Emotional Impact of Living with Chronic Endometriosis Pain
Living with chronic pain doesn’t just affect the body—it can take a toll on mental health, self-esteem, and relationships.
- Anxiety and Depression – Constant pain can lead to frustration, sadness, and feelings of helplessness. The unpredictability of flare-ups may cause fear of social activities or avoidance of certain situations.
- Impact on Intimacy and Relationships – Many people with endometriosis experience pain during intercourse (dyspareunia), which can create emotional distance or tension in relationships. Open communication and seeking support can help navigate these challenges.
- Self-Esteem and Identity – Struggling with pain and fatigue can make it difficult to engage in activities you once loved, leading to a loss of confidence and feelings of isolation.
Pain isn’t just physical—it affects the nervous system, emotions, and stress levels, all of which can make symptoms worse. A holistic approach that includes mental health support, relaxation techniques, and body awareness can help manage both the physical and emotional aspects of endometriosis pain.
How to Manage Endometriosis Pain Without Surgery
There’s no one-size-fits-all approach to managing endometriosis pain, but a combination of medical and supportive treatments could make a significant difference in improving your quality of life.
Medical Treatment Options for Endometriosis
- Hormone Therapy: Birth control pills, IUDs, and GnRH agonists can help regulate or suppress ovulation, reducing endometrial tissue growth and alleviating pain.
- Pain Medications: Over-the-counter NSAIDs (like ibuprofen) or prescription pain relievers may provide relief during flare-ups.
- Surgical Options: In severe cases, laparoscopy or excision surgery can remove excess endometrial tissue to reduce pain. A hysterectomy may also be an option, where the uterus is removed, eliminating the source of endometrial tissue growth. This prevents further inflammation, scarring, and adhesions caused by conditions like endometriosis or adenomyosis. With the uterus gone, menstrual cycles stop, reducing pain from cramping and abnormal tissue growth.
How Pelvic Floor Physical Therapy Helps Endometriosis Pain
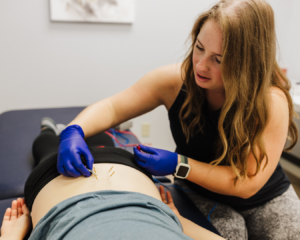
Dry needling and electronic stimulation can target back pain from endometriosis, offering effective relief from chronic discomfort.
- Pelvic Floor Physical Therapy: Many individuals with endometriosis develop pelvic floor dysfunction due to chronic pain and muscle guarding. Physical therapy can help by:
- Releasing muscle tension in the pelvic floor, abdomen, and lower back
- Improving posture and core stability to reduce pressure on the pelvic organs
- Teaching relaxation techniques to break the cycle of pain and muscle tightness
- Acupuncture, Dry Needling, and Massage Therapy: These therapies can help increase blood flow, reduce inflammation, and decrease nerve sensitivity, promoting overall relaxation.
- Dietary Changes: Certain foods may trigger inflammation, while others can help reduce it.
If you’re looking for endometriosis pain relief in San Antonio, know that there are effective, evidence-based options available — from medical care to pelvic floor therapy — to help you take control of your symptoms.
Lifestyle Changes for Living with Endometriosis
Making small lifestyle changes can have a big impact on managing pain and preventing flare-ups.
Exercise Modifications
High-impact activities, like running or intense weightlifting, may worsen symptoms. Instead, try lower-impact exercises like yoga, Pilates, walking, or swimming. Focus on gentle movements and incorporate breathwork and stretching to improve flexibility and circulation.
Managing Stress and Pain Exacerbation
Chronic pain can keep the nervous system in a constant “fight or flight” state, which can amplify symptoms. Try these approaches to manage stress and support your body:
- Diaphragmatic breathing: Helps calm the nervous system and relax the pelvic floor.
- Mindfulness and meditation: A great way to manage pain perception and reduce stress.
- Counseling or support groups: Seek emotional support and coping strategies from professionals or peers.
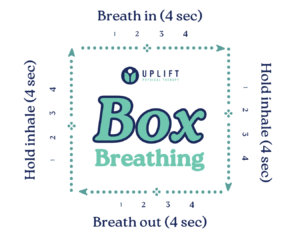
Calm your mind and body with box breathing—an easy-to-follow technique to manage pain and stress from endometriosis.
Anti-Inflammatory Nutrition
Your diet plays a key role in managing inflammation and hormone balance, both of which impact endometriosis symptoms.
- Consider adding more Omega-3 fatty acids, leafy greens, turmeric, ginger, and fiber-rich foods to your diet.
- Avoid processed foods, refined sugars, dairy, gluten, and alcohol (especially if they trigger symptoms).
Finding the Right Endometriosis Support in San Antonio
Living with endometriosis doesn’t mean you have to navigate it alone. Endometriosis is complex, and managing the condition requires a personalized, multi-faceted approach to pain management.
- Gynecologist: A specialist in endometriosis can assist with diagnosis, medical treatment options, and surgery when necessary.
- Pelvic Floor Therapist: A therapist can help with muscle dysfunction, pain management, and restoring mobility from inflammation or adhesions.
- Mental Health Professional: Living with chronic pain affects emotional well-being, and a counselor can help with coping strategies and provide essential emotional support.
Pain management is absolutely possible with the right support system and a proactive approach. Whether it’s through medical treatments, lifestyle changes, or holistic therapies, there are many options to help you take control of your health. Advocate for yourself, seek knowledgeable providers, and don’t settle for persistent pain being dismissed as “normal.” By finding the right treatment plan, you can improve your daily function, reduce discomfort, and reclaim a more fulfilling life.
At UpLift, we work with endometriosis pain relief San Antonio. We create customized treatment plans that address both the physical and emotional aspects of chronic pain. If you’re struggling with pelvic pain, urinary symptoms, or pain with intercourse, pelvic floor therapy can restore function, improve mobility, and reduce discomfort.
Endometriosis Pain Relief FAQs
“Can dry needling and/or cupping help relieve endometriosis pain?”
Yes, both dry needling and cupping can be effective in managing muscle tension and myofascial pain related to endometriosis. While these treatments do not directly treat endometriosis, they can help alleviate secondary muscle pain and improve mobility.
- Dry needling targets trigger points in tight muscles, particularly in the pelvic floor, abdomen, lower back, and hips, which often become tense due to chronic pain and inflammation. It can help release tightness, improve blood flow, and reduce pain sensitivity.
- Cupping therapy uses suction to increase circulation and reduce fascial restrictions. It may help relieve abdominal bloating, scar tissue tightness (from surgeries like C-sections or laparoscopy), and musculoskeletal pain.
“Can endometriosis cause weight gain or bloating?”
Yes, many people with endometriosis experience bloating, fluid retention, and weight fluctuations due to:
- Inflammation: Chronic inflammation can cause bloating and fluid retention, often referred to as “endo belly.”
- Hormonal imbalances: Endometriosis is an estrogen-driven condition, and excess estrogen may contribute to weight gain, bloating, and digestive issues.
- Digestive disruptions: Many individuals with endometriosis experience IBS-like symptoms, such as constipation, gas, and bloating.
- Medications and treatments: Hormonal therapies (like birth control or GnRH agonists) may cause water retention or metabolic changes that affect weight.
Lifestyle changes such as an anti-inflammatory diet, pelvic floor therapy, and gut health support can help manage these symptoms.
“Will endometriosis go away after menopause?”
Not always. While menopause leads to a natural decline in estrogen levels, which may reduce symptoms, some individuals continue to experience pain due to:
- Existing scar tissue and adhesions: Even after estrogen levels drop, adhesions and scarring from endometriosis can continue to cause pain.
- Estrogen production from other sources: The body still produces a small amount of estrogen after menopause, which may trigger symptoms.
- Postmenopausal hormone therapy (HRT): Some people take HRT to manage menopause symptoms, but it may reactivate endometriosis symptoms in certain cases.
“What positions are best for managing endometriosis pain during sex?”
Endometriosis can cause discomfort during sex due to the presence of endometrial tissue outside the uterus. To minimize pain, consider the following:
- Communication: Discuss with your partner what feels comfortable and what doesn’t.
- Positions: Positions that allow you to control the depth and angle of penetration, such as being on top, may reduce discomfort.
- Lubrication: Using a water-based lubricant can decrease friction and alleviate pain (we recommend Good Clean Love or Slipper Stuff).
- Timing: Engaging in sex when you’re experiencing the least amount of pain, such as after a warm bath or during certain times of your menstrual cycle, might be beneficial.
Everyone’s experience with endometriosis is unique, so it’s important to find what works best for you.
You can read more about managing pain with sex in our blog here!
“Can I live a normal life with endometriosis?”
Yes, many individuals with endometriosis can lead fulfilling lives through various strategies:
- Medical treatment: Options include pain relievers, hormonal therapies, and, in some cases, surgery.
- Lifestyle adjustments: Regular exercise, a balanced diet, and adequate rest can help manage symptoms.
- Support systems: Connecting with support groups or counseling can provide emotional relief and practical advice. Work closely with your healthcare provider to develop a personalized management plan that addresses your specific needs.
“How can I cope with the emotional toll of living with endometriosis pain?”
- Seek support: Join support groups to share experiences and gain insights from others facing similar challenges.
- Professional help: Consider counseling or therapy to develop strategies for managing pain and emotional stress.
At UpLift, we specialize in endometriosis pain relief in San Antonio, combining medical treatment and pelvic floor therapy to help women move with greater comfort and confidence.
Wrapping Up
Endometriosis is often misunderstood, but you don’t have to face it alone. With the right combination of medical care, pelvic floor therapy, lifestyle modifications, and emotional support, it is possible to manage pain and improve your quality of life.
If you’re struggling with pelvic pain, bladder issues, or painful intercourse, seeking treatment from a team of professionals who understand endometriosis can be life-changing. There is hope, and there are solutions. By listening to your body, advocating for yourself, and exploring different treatment options, you can take control of your health and move toward a future with less pain and more freedom.
If you are seeking endometriosis pain relief in San Antonio, a holistic approach that combines medical treatment, pelvic floor therapy, and lifestyle changes can make a significant difference in daily comfort and long-term well-being.
Contact Us
Have questions or want to learn more about how physical therapy can help you manage your endometriosis symptoms? Reach out—UpLift is here to guide you through your pelvic floor journey!

